In the clinic, I often hear patients say, “Doctor, my cholesterol is normal, so I don’t need to worry about my heart, right?”
It’s a common belief. For decades, we’ve been trained to look at cardiovascular health through a few familiar numbers. We assume that if our blood pressure is stable and our lipids are low, we are in the clear.
However, modern clinical science is revealing a deeper truth: Cardiovascular disease isn’t just a “fat” problem—it is driven by a hidden engine of chronic inflammation.
What is hsCRP? The Body’s “Systemic Broadcast”
High-sensitivity C-reactive protein (hsCRP) is a protein produced by the liver. It isn’t a hormone or an immune cell; think of it as a broadcast signal for systemic inflammation.
Whenever there is tissue damage, oxidative stress, or immune irritation anywhere in the body, immune signaling molecules (specifically Interleukin-6) tell the liver to start churning out this protein. Therefore, this number doesn’t point to one specific organ; it reflects the current state of your entire immune system.
Many people mistake hsCRP for a passive bystander. In molecular medicine, we know it is an active participant in disease. Under chronic low-grade inflammation, hsCRP actively interferes with your vascular system:
- Vascular Lining: It makes immune cells “sticky,” causing them to adhere to vessel walls.
- Immune Amplification: It keeps the immune system on high alert, preventing the body from entering a “repair” mode.
- Lipid Oxidation: It promotes the formation of oxidized LDL, accelerating the creation of plaque.
- Energy Failure: It impairs mitochondrial function, reducing the ability of vascular cells to heal themselves.
This doesn’t happen overnight. It’s a slow accumulation of damage—arteries lose elasticity, plaques become unstable, and eventually, this leads to a heart attack or stroke.
The 2025 Study: A Crystal Ball for Heart Health
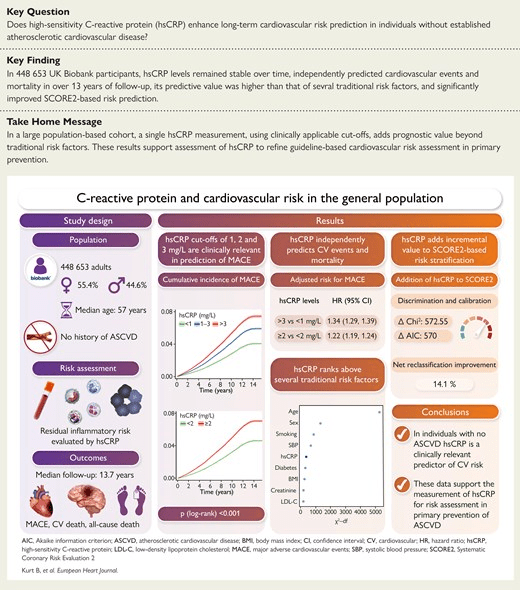
A landmark study published in the European Heart Journal (2025) analyzed 448,653 adults with no prior history of heart disease, following them for over 13 years. The researchers categorized hsCRP levels into three risk tiers:
- Low Risk: $< 1$ mg/L
- Moderate Risk: $1 – 3$ mg/L
- High Risk: $> 3$ mg/L
The results were a wake-up call. Compared to those in the “Low Risk” group, individuals with hsCRP $> 3$ mg/L saw:
- 34% increase in major cardiovascular events.
- 61% increase in cardiovascular death.
- 54% increase in all-cause mortality.
In short, a high hsCRP isn’t just “slightly elevated”—it correlates with a more than 50% increase in the risk of death.
The Key Takeaway: While cholesterol tells us how much “oil” is in the system, hsCRP tells us if the “engine is overheating.” Studies suggest hsCRP can be 2 to 3 times more predictive of future heart events than LDL cholesterol alone.
High inflammation is rarely a single-issue problem. It is usually a “molecular shift” involving several systems:
- Oxidative Stress: The body’s cleanup crew can’t keep up with metabolic waste.
- Fatty Acid Imbalance: Diets high in pro-inflammatory oils.
- Chronic Stress: Elevated stress hormones dysregulate the autonomic nervous system.
- Gut Health: A compromised gut barrier keeps the immune system in a state of constant irritation.
Your body knows when this is happening. You might feel chronically tired, have fluctuating moods, sensitive digestion, or notice that you take longer to recover after exercise. These aren’t random symptoms; they are the signals of a system under inflammatory load.
How to “Cool Down” the Inflammation
The goal isn’t to “fix” the number with a pill, but to shift the body’s internal environment:
- Prioritize Circadian Health: Consistent sleep schedules allow stress hormones to drop, giving the immune system a chance to reset.
- Intermittent Gut Rest: Avoid constant grazing. Reducing the frequency of food intake (and cutting out ultra-processed sugars) lowers the daily “immune burden” on your gut.
- Mitochondrial Recovery: Instead of high-intensity “grind” workouts, focus on low-to-moderate intensity movement that your body can actually recover from.
- Anti-Inflammatory Nutrition: Shift your fat intake toward Omega-3s and antioxidant-rich whole foods to change the molecular structure of your cells.
Here are some Top Anti-Inflammatory Food Groups:
- Fruits: Berries (blueberries, strawberries), cherries, citrus fruits, and oranges.
- Vegetables: Dark leafy greens (kale, spinach, Swiss chard), broccoli, cabbage, and peppers.
- Healthy Fats & Oils: Extra virgin olive oil, avocado, and nuts like walnuts and almonds.
- Fatty Fish: Salmon, mackerel, sardines, and anchovies, which are high in omega-3 fatty acids.
- Spices & Herbs: Turmeric, ginger, garlic, and cinnamon.
- Whole Grains: Oats, quinoa, brown rice, and buckwheat.
- Legumes & Seeds: Lentils, black beans, chia seeds, and flaxseed.
- Other: Green tea, dark chocolate, and fermented foods like kefir or sauerkraut.

Heart disease isn’t a sudden accident; it’s the result of molecular systems moving in the wrong direction for years.
The beauty of the hsCRP marker is that it allows us to see the “hidden fire” before the building burns down. It gives us the power to change direction while the damage is still reversible.
Understanding your “internal weather” is the first step toward a longer, healthier life. If you found this helpful, feel free to share it with someone who only looks at their cholesterol!
Source: https://academic.oup.com/eurheartj/advance-article/doi/10.1093/eurheartj/ehaf937/8377304